Intro
Week 12 of pregnancy often feels like a meaningful threshold. You are nearing the end of the first trimester, a period when the foundations of fetal anatomy have been laid down and many people begin to notice subtle shifts in symptoms, energy, and body shape. It can be a hopeful time, but it may also bring anxiety, especially if you are waiting for scan results, screening tests, or reassurance that everything is progressing as expected.
At 12 weeks, the fetus is still very small, yet remarkably complex. Facial features are becoming more defined, fingernails are forming, and internal organs continue to mature. For the pregnant person, the placenta is increasingly taking over hormone production, which may help explain why nausea and fatigue start to ease for some. As always, experiences vary widely, and any concerns should be discussed with a midwife, obstetrician, family physician, or other qualified maternity care professional.
Highlights
Week 12 is commonly considered the final week of the first trimester, marking a transition from early embryonic development into ongoing fetal growth and maturation.
The fetus has a more recognizable profile, developing fingernails, and intestines that move into the abdomen as development progresses.
Many people notice that nausea, breast tenderness, and fatigue begin to improve around this stage, although symptoms can continue or fluctuate.
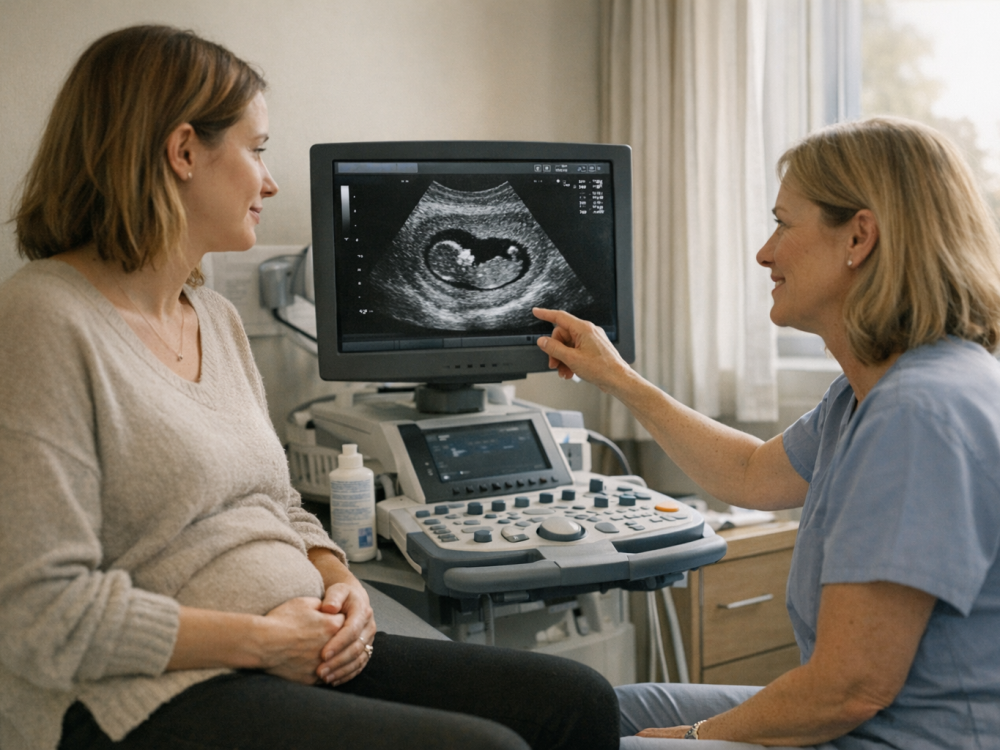
This is often the time for first-trimester ultrasound dating and screening discussions, depending on local care pathways and individual circumstances.
New or severe symptoms, especially heavy bleeding, significant pain, fainting, or fever, should prompt urgent medical advice.
Why week 12 is a milestone
Pregnancy is usually dated from the first day of the last menstrual period, even though conception typically occurs about two weeks later in a 28-day cycle. By week 12, you are approaching the end of the first trimester, a phase characterized by rapid cell division, organ formation, and major structural development. The term fetus is used after the embryonic period, and by this stage the body plan is established while organs continue to grow and mature.
This transition can feel psychologically important. Many people associate the end of the first trimester with a reduction in early pregnancy uncertainty, though it is important to remember that risk does not disappear and every pregnancy is individual. If you have a history of miscarriage, fertility treatment, pregnancy complications, or significant anxiety, week 12 may bring mixed feelings rather than simple relief. Compassionate support and clear communication with your care team can make this stage easier to navigate.
Fetal development at 12 weeks
By the end of week 12, fetal development is increasingly detailed. According to major clinical pregnancy references, the fetus has a more developed facial profile, and small structures such as fingernails are forming. The intestines, which develop partly outside the abdominal cavity early in pregnancy, move into the abdomen as the body grows. These changes reflect the transition from early structural formation toward refinement, growth, and functional maturation.
The fetus is still too small for movements to be felt by most pregnant people, but spontaneous movement may be visible on ultrasound. The head remains proportionally large compared with the rest of the body, and facial features are becoming more recognizable. Limb development continues, and the skeleton is gradually changing as cartilage begins the long process of ossification, or bone formation.
At this stage, fetal sex organs are developing, but external genital appearance may not be reliably determined on all scans. Accuracy depends on fetal position, gestational age, equipment quality, and the expertise of the person scanning. If you are hoping to learn fetal sex, your clinician can explain when and how that information may be most reliable in your setting.
Changes in your body: symptoms that may shift
Many people find that early pregnancy symptoms begin to ease around 12 weeks, although this is not universal. Nausea and vomiting may lessen as placental hormone support becomes more established, and some people notice a gradual return of appetite and energy. Others continue to feel unwell for several more weeks, and a minority experience severe nausea and vomiting, known as hyperemesis gravidarum, which requires medical assessment and support.
Common changes around this time can include:
- Less intense nausea or food aversions, though symptoms may still come and go.
- Ongoing fatigue, sometimes improving slowly rather than suddenly.
- Breast enlargement, tenderness, or visible veins due to hormonal and circulatory changes.
- A thickening waist or bloating, even if a clear bump is not yet visible.
- More frequent urination, constipation, heartburn, or mood changes.
A sudden change in symptoms does not automatically mean something is wrong. Symptoms naturally fluctuate. However, if symptom changes are accompanied by bleeding, cramping, dizziness, fever, severe pain, or a general feeling that something is not right, contact your maternity care provider for guidance.
The placenta and hormonal support
A key physiological development near the end of the first trimester is the placenta’s increasing role in sustaining the pregnancy. Early on, the corpus luteum in the ovary provides essential progesterone support. As pregnancy progresses, the placenta becomes a major endocrine organ, producing hormones that help maintain the uterine lining, support fetal growth, and adapt maternal metabolism.
This shift may be one reason some people feel better after the first trimester, although hormone levels remain high and can still produce symptoms. Progesterone can slow gastrointestinal motility, contributing to constipation and reflux. Human chorionic gonadotropin, estrogen, and other placental hormones influence nausea, breast changes, vascular tone, and emotional sensitivity. These changes are physiological, but that does not make them easy. If symptoms interfere with hydration, nutrition, sleep, work, or mental wellbeing, professional help is appropriate.
Appointments, ultrasound, and screening conversations
Week 12 often falls within the window for first-trimester assessment, though timing varies by country, health system, and individual risk factors. Many people have a dating ultrasound around this period to confirm gestational age, check fetal heartbeat, assess the number of fetuses, and estimate the due date. Ultrasound findings should always be interpreted by qualified professionals in the context of your full clinical picture.
You may also be offered screening for chromosomal conditions. Depending on your location and medical history, this might include combined first-trimester screening, nuchal translucency measurement, maternal blood tests, or non-invasive prenatal testing, often called NIPT. Screening tests estimate risk; they do not usually provide a definitive diagnosis. If a screening result indicates increased risk, your clinician may discuss diagnostic testing options such as chorionic villus sampling or amniocentesis, including their benefits, limitations, and potential risks.
This is also a good time to review routine prenatal topics: blood group and rhesus status, anemia screening, infection screening, medications and supplements, vaccination recommendations, lifestyle risks, and any chronic conditions such as thyroid disease, diabetes, hypertension, epilepsy, autoimmune disease, or mental health concerns. If you take prescription, over-the-counter, or herbal products, do not stop or start them without medical advice.
Nutrition, supplements, and everyday self-care
At 12 weeks, practical self-care remains important, but it should be realistic. If you have been struggling with nausea or food aversions, your diet may not feel ideal. Focus on hydration, tolerable nutrient-dense foods, and gradual improvement rather than perfection. Small, frequent meals may be easier than large meals, and bland foods can be helpful during nausea flares.
General priorities to discuss with your healthcare professional include:
- Folic acid or prenatal vitamins, according to your clinical situation and local guidance.
- Vitamin D, iodine, iron, or other supplements only where recommended or appropriate.
- Food safety measures, including avoiding high-risk foods for listeria or toxoplasmosis where relevant.
- Limiting caffeine within recommended local thresholds and avoiding alcohol and smoking.
- Gentle physical activity if safe for you, such as walking, swimming, or prenatal yoga.
Some people feel ready to become more active as fatigue improves. Others need more rest. If you have bleeding, significant pain, placenta-related concerns, cervical problems, severe anemia, heart or lung disease, or a high-risk pregnancy, ask your clinician what activity level is safe for you.
Emotional wellbeing and sharing the news
The end of the first trimester is often when people begin deciding whether to share pregnancy news more widely. There is no correct timeline. Some prefer early support from family, friends, or colleagues; others wait until after ultrasound or screening results. Your decision may depend on your privacy needs, workplace considerations, cultural expectations, previous pregnancy experiences, or simply what feels emotionally safe.
Anxiety at 12 weeks is common, especially if symptoms lessen before you have confirmation that the pregnancy is progressing. It can help to write down questions before appointments, ask what changes should prompt urgent care, and clarify how to contact your maternity unit between visits. If worry becomes intrusive, affects sleep or appetite, or triggers panic, consider speaking with a healthcare professional. Mental health is part of prenatal health, not an afterthought.
When symptoms need prompt medical advice
Most mild aches, bloating, and symptom fluctuations are part of normal pregnancy physiology, but some symptoms require timely assessment. Contact your healthcare provider, urgent care service, or emergency department according to local guidance if you experience heavy bleeding, severe abdominal or pelvic pain, shoulder tip pain, fainting, severe dehydration, fever, or signs of infection. If you have a known medical condition or high-risk pregnancy, your threshold for seeking advice may be lower.
It is better to ask and be reassured than to wait with symptoms that worry you. Healthcare professionals are used to evaluating early pregnancy concerns and can advise whether monitoring, examination, blood tests, ultrasound, or urgent care is needed.
Seek medical advice urgently if
- You have heavy vaginal bleeding, clots, or bleeding with significant pain.
- You develop severe abdominal or pelvic pain, shoulder pain, fainting, or dizziness.
- You cannot keep fluids down or have signs of dehydration.
- You have fever, chills, painful urination, or symptoms of infection.
- You feel unsafe, severely anxious, or at risk of harming yourself.
Tools & Assistance
- Prepare a question list for your 12-week appointment or ultrasound visit.
- Keep a symptom and medication record to share with your midwife or clinician.
- Use your maternity unit, obstetric clinic, or primary care service for non-urgent concerns.
- Contact emergency services or urgent maternity triage for severe bleeding, pain, fainting, or dehydration.
- Ask your care team about local prenatal screening options and what each result can and cannot tell you.
FAQ
Is week 12 the end of the first trimester?
Week 12 is commonly treated as the final week of the first trimester, with the second trimester beginning around week 13. Dating conventions can vary slightly, so your clinician may use a specific system.
Should my nausea be gone by 12 weeks?
It may improve around this time, but it does not disappear for everyone. If vomiting is severe, you cannot stay hydrated, or weight loss is occurring, contact a healthcare professional.
Can I feel the baby move at 12 weeks?
Fetal movement may occur, but it is usually too early for most pregnant people to feel it. First movements are typically felt later, often in the second trimester.
What might be seen on a 12-week ultrasound?
A scan may assess gestational age, heartbeat, fetal number, and basic anatomy appropriate for this stage. Some settings also measure nuchal translucency as part of screening.
Is it safe to announce pregnancy after 12 weeks?
The timing is a personal choice. Some people feel more comfortable after early screening or ultrasound, while others share earlier or later depending on their support needs and privacy.
Sources
- Mayo Clinic — Fetal development: The first trimester
- NHS — 12 weeks pregnant guide - Best Start in Life
- MedlinePlus — Fetal development: Milestone chart
Disclaimer
This article is for general educational information only and does not replace personalized medical advice. Always consult a qualified healthcare professional about pregnancy symptoms, screening decisions, medications, or concerns.