Intro
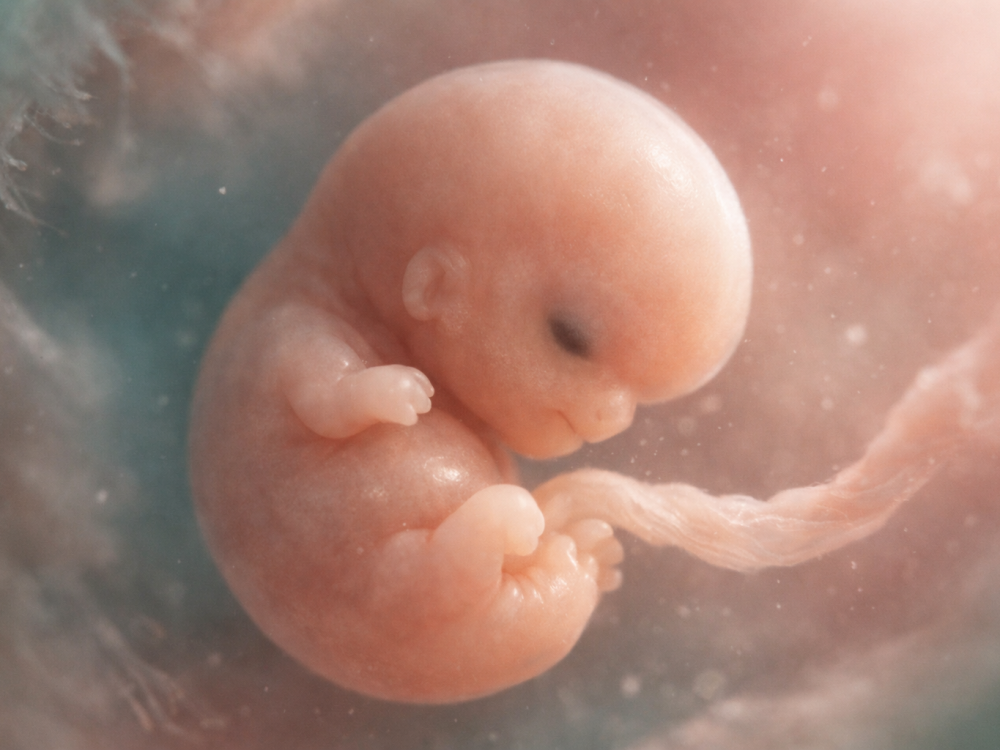
Week 7 of pregnancy is often a surprisingly intense time: the embryo is still tiny, yet development is moving at extraordinary speed. Many people are coping with nausea, fatigue, breast tenderness, heightened smell, mood changes, or anxiety while also trying to absorb the reality that major organs and body structures are taking shape.
At this stage, pregnancy dating is usually counted from the first day of the last menstrual period, so week 7 corresponds to about five weeks after conception. The embryo is around 10 mm long according to NHS guidance, but the pace of change is remarkable: the brain is growing rapidly, early facial features are emerging, and limb buds are beginning to form the framework of arms and legs.
Highlights
The embryo is approximately 10 mm long at week 7, yet brain, face, and limb development are progressing quickly.
Rapid neural development is a central feature of this week, with early connections and central nervous system organization beginning in a head-to-tail sequence.
Facial structures such as early eye regions, nose dimples, nostril areas, and ear formation are becoming more defined.
Arm and leg buds are present, and cartilage is beginning to form as the early template for future bones.
Maternal symptoms can be strong because hormonal and circulatory changes are supporting rapid embryonic growth.
How big is the embryo at week 7?
By week 7 of pregnancy, the embryo is still very small, measuring around 10 mm in length according to the NHS week-by-week pregnancy guide. Size can vary, and ultrasound measurements are interpreted in context by healthcare professionals, especially because ovulation and implantation timing can differ from one person to another.
Despite its small size, this is a period of rapid morphogenesis, meaning the embryo’s overall body plan and organ systems are developing in a highly coordinated way. The head is proportionally large because the brain and cranial structures are growing quickly. The trunk is lengthening, the early spinal region is developing, and the beginnings of the upper and lower limbs are becoming visible as limb buds.
For many pregnant people, this contrast can feel astonishing: the embryo is only about the size of a small berry, yet development is not simple or passive. Cells are proliferating, migrating, differentiating, and communicating through tightly regulated molecular signals. This is one reason early pregnancy care focuses on folic acid, avoiding harmful exposures, and seeking individualized medical guidance when medications, chronic conditions, or previous pregnancy complications are relevant.
Rapid brain growth and early nervous system activity
Week 7 is a particularly important period for the developing nervous system. The NHS notes that the brain is growing rapidly at this stage, producing around 100 new brain cells per minute. This figure helps illustrate the speed of neurodevelopment, although the developing brain is still far from mature and will continue to grow and organize throughout pregnancy, infancy, childhood, and adolescence.
The central nervous system develops in a staged pattern. Earlier in embryonic life, the neural tube forms and gives rise to the brain and spinal cord. Around week 7 of gestation, evidence-based developmental descriptions note that the first synapses are forming in the spinal cord approximately five weeks after conception. Synapses are communication points between nerve cells, and their emergence represents the beginning of organized neural signaling. Development proceeds from the spinal cord upward toward more complex brain regions over time.
It is important to interpret this carefully. Early neural activity is not the same as conscious thought, sensation in the mature sense, or awareness. Rather, it reflects the earliest biological infrastructure of the nervous system: cells forming circuits, establishing connections, and preparing for later functions. Much of what people think of as brain function depends on later maturation of the cerebral cortex, sensory pathways, thalamocortical connections, and postnatal experience.
For a medically literate reader, week 7 can be understood as a time of intense neurogenesis, early patterning, and primitive synaptogenesis. This makes routine prenatal care and risk reduction important, but it should not become a source of self-blame. Many developmental processes are resilient, and if you have concerns about medication exposure, infection, alcohol, nutrition, or another factor, the safest next step is to discuss it promptly with a qualified clinician rather than trying to assess risk alone.
Face formation: eyes, nose, ears, and early mouth structures
The face begins to look more complex during week 7, although it is still in a very early embryonic form. NHS guidance describes nose dimples and eye development at this stage. Other clinical pregnancy resources describe the emergence of early facial features including the eyes, nostril areas, and ears.
Facial development is a coordinated process involving tissue growth, folding, and fusion. The early eye regions are forming on the sides of the head before gradually moving toward a more forward-facing position later in development. The small depressions that contribute to nasal structures become more recognizable, and the ear primordia begin forming in their early positions before later remodeling and migration.
The mouth and jaw region are also developing, shaped by embryonic facial prominences. These structures will continue to remodel over many weeks. At this stage, they do not resemble a newborn’s face, but the biological foundations are being laid. Because facial development depends on precise timing, clinicians may ask about folic acid use, medical history, medication exposures, diabetes control, and other factors during early pregnancy appointments. These conversations are not meant to alarm you; they help tailor care and identify preventable risks where possible.
If you are waiting for a first scan, it is normal to feel impatient or nervous. At week 7, ultrasound may sometimes identify an intrauterine pregnancy and cardiac activity depending on timing, equipment, and individual circumstances, but interpretation should always be done by trained healthcare professionals. If dates are uncertain, a repeat scan may be recommended rather than assuming something is wrong.
Limb buds and the cartilage framework for future bones
During week 7, the arm and leg buds are developing. These limb buds are small protrusions that will gradually form the upper and lower limbs. The NHS describes limb bud formation and cartilage development for bones at this stage, meaning the embryo is beginning to create the early template that will later undergo ossification, the process by which bone tissue forms.
Cartilage is essential in early skeletal development because it provides a flexible scaffold. Over time, many of these cartilage models are replaced by bone, while some cartilage remains in joints and growth regions. The process is gradual and continues well beyond the first trimester.
The upper limbs generally develop slightly ahead of the lower limbs. In the coming weeks, early hand and foot plates will become more distinct, and digital rays will contribute to finger and toe formation. At week 7, however, the limb structures are still primitive. Movement may begin as simple reflexive activity later, but it is far too early for the pregnant person to feel fetal movement.
If you are thinking ahead to future scans, detailed assessment of limbs and anatomy is usually performed later in pregnancy, commonly at the mid-pregnancy anomaly scan depending on local healthcare systems. Early scans may provide important information about viability, location, dating, and number of embryos, but they cannot evaluate all structures in detail at week 7.
What you may feel in your body this week
While the embryo is undergoing rapid development, your body is adapting through substantial hormonal, vascular, and metabolic changes. Rising human chorionic gonadotropin, progesterone, and estrogen contribute to many early pregnancy symptoms. Thomson Medical describes maternal physiological changes such as uterine expansion and hormonal shifts that support fetal growth.
Common symptoms around week 7 can include nausea or vomiting, fatigue, breast tenderness, bloating, food aversions, constipation, mild cramping, increased urination, emotional sensitivity, and heightened sense of smell. Some people have many symptoms; others have few. Symptom intensity alone does not reliably indicate whether a pregnancy is healthy.
Mild uterine cramping can occur as the uterus begins to change, but severe pain, one-sided pelvic pain, heavy bleeding, shoulder-tip pain, fainting, or feeling very unwell should be assessed urgently because they can signal complications such as ectopic pregnancy or significant bleeding. If you are unsure whether a symptom is concerning, it is reasonable to contact your maternity unit, obstetric clinician, midwife, primary care professional, or local urgent care service.
Nausea can be especially difficult at this point. General supportive measures may include small frequent meals, hydration, avoiding triggers, and rest. However, persistent vomiting, inability to keep fluids down, reduced urination, dizziness, or weight loss may indicate dehydration or hyperemesis gravidarum and deserves medical review. Safe treatment options exist, but they should be discussed with a clinician who knows your medical history.
Prenatal care priorities at week 7
Week 7 is a good time to ensure you are connected with prenatal care, particularly if you have not already contacted a healthcare professional. Depending on your country and healthcare system, this may involve a midwife booking appointment, obstetric visit, primary care appointment, early pregnancy clinic, or referral for ultrasound if clinically indicated.
Key topics to raise with a professional include current medications and supplements, chronic conditions such as diabetes, epilepsy, hypertension, thyroid disease, autoimmune disease, mental health conditions, previous pregnancy loss or complications, occupational exposures, and any bleeding or pain. Do not stop prescribed medication abruptly unless a clinician advises you to, because untreated maternal illness can also carry pregnancy risks.
- Confirm whether you are taking the recommended folic acid dose for your circumstances; some people need a higher prescribed dose.
- Ask about vitamin D, iodine, iron, or other supplements if relevant to your diet, location, or medical history.
- Discuss food safety, alcohol, smoking, vaping, recreational drugs, and workplace exposures in a nonjudgmental clinical setting.
- Clarify when your first ultrasound or booking appointment should occur.
- Seek support early if anxiety, low mood, trauma history, or pregnancy after loss is affecting your wellbeing.
Good prenatal care is not only about detecting problems. It is also about reassurance, planning, and making sure you have a reliable route for questions as pregnancy progresses.
Emotional wellbeing during a fast-changing stage
The science of week 7 can be fascinating, but the lived experience may be messy. You may feel excited one moment and frightened the next. You may also feel detached, especially if you have had previous loss, fertility treatment, or a long period of trying to conceive. All of these reactions are common and understandable.
Because early pregnancy is often invisible to others, symptoms can feel isolating. You may be working, caring for other children, studying, or managing responsibilities while feeling exhausted or nauseated. Practical support can make a real difference: letting a trusted person know, adjusting routines where possible, keeping snacks and fluids nearby, and prioritizing sleep are simple but meaningful steps.
If worry becomes intrusive, if you feel persistently low, or if you are struggling to function, reach out to a healthcare professional. Perinatal mental health support can begin in the first trimester; you do not have to wait until later pregnancy. Emotional care is part of medical care.
Seek medical advice urgently if you notice
- Heavy vaginal bleeding, passing large clots, or bleeding with severe pain.
- Severe or one-sided pelvic pain, shoulder-tip pain, fainting, or collapse.
- Persistent vomiting, inability to keep fluids down, dizziness, or very reduced urination.
- Fever, severe abdominal pain, or feeling acutely unwell.
- Any symptom that worries you, especially with a history of ectopic pregnancy, miscarriage, or fertility treatment.
Tools & Assistance
- Contact your midwife, obstetrician, primary care clinician, or early pregnancy unit for personalized guidance.
- Keep a symptom diary noting bleeding, pain, vomiting, hydration, medications, and questions for appointments.
- Review all prescription, over-the-counter, and herbal products with a healthcare professional.
- Use trusted pregnancy week-by-week resources from recognized medical organizations.
- Seek urgent care or emergency services if you have severe pain, heavy bleeding, fainting, or signs of dehydration.
FAQ
Is the baby’s brain already working at week 7?
Early nervous system activity is beginning, including the formation of first synapses in the spinal cord around this stage. This is early biological signaling, not mature awareness or fully developed brain function.
Can I feel the embryo move at week 7?
No. Limb buds are developing, but the embryo is far too small and early movements are not felt. Most people feel fetal movement much later in pregnancy.
Is it normal to have strong nausea at week 7?
Yes, nausea is common in early pregnancy and may be intense. However, persistent vomiting, dehydration, dizziness, weight loss, or inability to keep fluids down should be discussed with a clinician.
What facial features are forming now?
Early eye regions, nose dimples or nostril areas, ear structures, and mouth or jaw foundations are developing, though the face remains very embryonic in appearance.
Should I be worried if my symptoms come and go?
Symptoms often fluctuate and do not reliably indicate pregnancy health. If you have bleeding, severe pain, fainting, or significant concern, contact a healthcare professional.
Sources
- NHS — 7 weeks pregnant guide - Best Start in Life
- Thomson Medical — Week 7 Pregnancy: Your Baby's Face Begins to Form
- Zero to Three — When does the fetus's brain begin to work?
Disclaimer
This article is for general educational information only and does not replace medical advice, diagnosis, or treatment. Always consult a qualified healthcare professional about pregnancy symptoms, medications, risks, and personal care decisions.