Intro
Week 9 of pregnancy is a meaningful biological transition. By conventional obstetric dating, you are still in the first trimester, but development is shifting from the embryonic period into the fetal stage. This does not mean growth becomes less important; rather, the foundations of the major organ systems are now in place, and the next phase emphasizes rapid growth, refinement of structures, and increasingly coordinated movement.
For many pregnant people, week 9 can also feel physically intense. Hormonal changes may be peaking, nausea and fatigue can be prominent, and emotional fluctuations are common. If symptoms feel overwhelming or you are unsure what is normal for you, it is appropriate to contact a midwife, obstetrician, family physician, or other qualified healthcare professional.
Highlights
At around 9 weeks, the embryo is generally described as entering the fetal stage, with body systems continuing to mature and specialize.
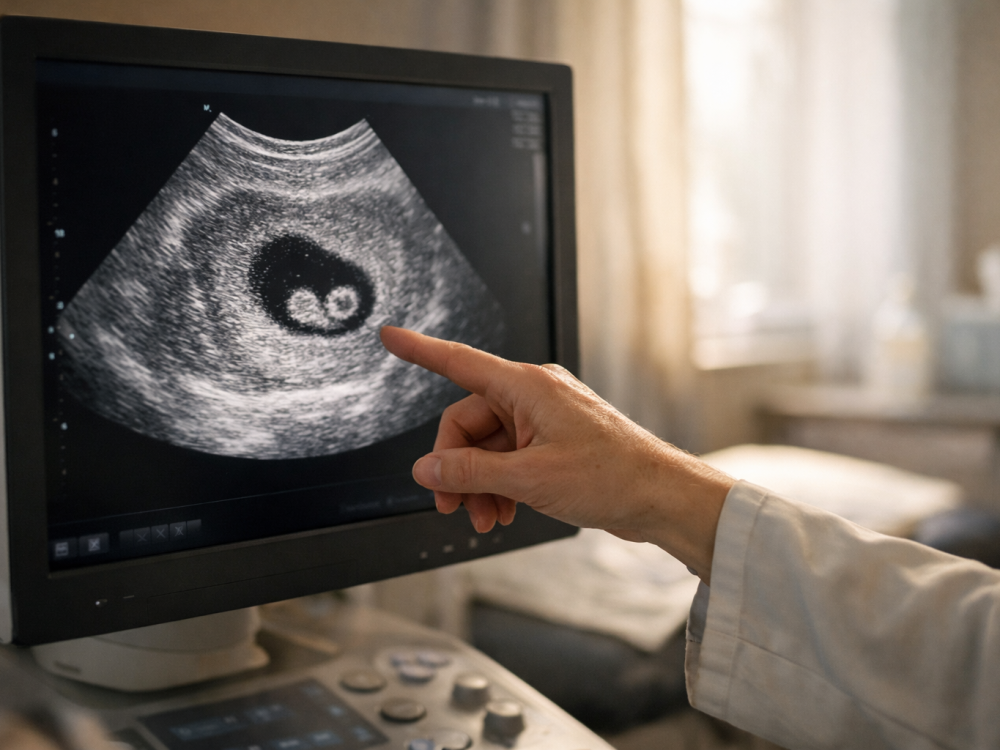
The fetus is small but rapidly developing: NHS describes it as approximately 22 mm long, around the size of a strawberry, while other references may use different measurement conventions.
Key structural changes include eyelid formation, tongue and early taste bud development, grooves that will become fingers and toes, joint formation, and the disappearance of the embryonic tail.
The heart is developing into a four-chambered structure with valves, and fetal heart rate may be very fast at this stage, reported by some developmental sources to peak around 170 beats per minute.
Maternal symptoms such as nausea, breast tenderness, fatigue, urinary frequency, bloating, and mood changes often reflect high levels of pregnancy hormones, but severe or worrying symptoms deserve medical review.
A major developmental milestone: from embryo to fetus
Week 9 marks the beginning of the fetal stage in many pregnancy week-by-week descriptions. During the earlier embryonic period, the central task is establishing the body plan and laying down the precursors of the major organs. In the fetal period, those structures continue to grow, mature, and become more recognizable and functional.
This distinction is important medically, but it should not create anxiety. Development is a continuum, and week 9 is still part of the first trimester, when organogenesis and early differentiation remain highly sensitive processes. The fetus is rapidly changing, and the placenta is continuing to take on an increasingly important role in hormone production and nutrient exchange.
Size estimates vary depending on whether crown-rump length, total length, or ultrasound conventions are being used. The NHS describes the fetus at week 9 as approximately 22 mm long, about the size of a strawberry. The American Pregnancy Association gives a measurement of about 1.67 inches from head to rump and notes that weight is still only a fraction of an ounce. These differences reflect measurement methods and dating variation rather than a single perfect standard for every pregnancy.
Body structure formation: head, face, eyelids, tongue, hands, and feet
By week 9, the fetal body is becoming more proportioned, although the head remains large relative to the body because the brain and cranial structures are growing quickly. The face continues to develop: eyelids are forming and may be fused, protecting the developing eyes for later stages. The tongue is developing, and early taste bud-like structures are emerging.
The limbs are also becoming more anatomically distinct. Grooves appear where fingers and toes will separate more clearly, and the beginnings of joints make movement possible. Knee and elbow joints are forming, and the fetus may begin small spontaneous movements involving the arms, hands, legs, and trunk. These movements are typically far too subtle to be felt by the pregnant person at this point.
Another visible developmental change is the disappearance of the embryonic tail. As the lower spine and pelvis mature, the tail-like structure seen earlier is no longer prominent. The torso lengthens, the neck becomes more defined, and the overall silhouette looks increasingly human in form, even though the fetus remains very small.
Heart, circulation, brain, and early movement
The cardiovascular system is undergoing rapid refinement. The fetal heart has developed a four-chambered structure, and valves are continuing to form. In early pregnancy, fetal heart rate is normally much faster than an adult heart rate. The Charlotte Lozier Institute describes the fetal heart rate as peaking around week 9 at approximately 170 beats per minute, nearly twice the maternal heart rate.
Brain development is equally dynamic. The cortex is expanding, and neural circuits are becoming more complex. These early neurological developments support spontaneous movement, although the movements are not yet purposeful in the way later fetal movements may appear. They are still important signs of neuromuscular maturation.
Because the fetus is so small and cushioned within the uterus, movement will not be felt this early. Most people first perceive fetal movement much later, often in the second trimester, with timing influenced by factors such as placental location, prior pregnancies, body habitus, and individual sensitivity.
What you may feel in your body at 9 weeks
Week 9 can be a demanding time physically. Human chorionic gonadotropin, progesterone, estrogen, and other pregnancy-related hormonal changes can contribute to nausea, food aversions, breast tenderness, fatigue, bloating, constipation, increased urination, headaches, and mood variability. Some people feel reassured by symptoms; others worry if symptoms fluctuate. Both experiences are common, and symptom intensity does not reliably measure pregnancy health.
Common experiences at this stage may include:
- Nausea or vomiting, often called morning sickness, though it can occur at any time of day
- Heightened sense of smell or sudden aversions to foods, drinks, or odors
- Breast fullness, tenderness, darker areolae, or visible veins
- Fatigue that feels disproportionate to activity level
- Mild pelvic heaviness or uterine stretching sensations
- Emotional sensitivity, anxiety, irritability, or tearfulness
Although many symptoms are physiologic, you do not need to simply endure them without support. Persistent vomiting, inability to keep fluids down, weight loss, dehydration symptoms, severe pain, fever, heavy bleeding, or fainting should be discussed promptly with a healthcare professional.
Prenatal care, screening, and dating at this stage
If you have not already arranged prenatal care, week 9 is a good time to do so. Early appointments often review medical history, medications and supplements, previous pregnancies, family history, lifestyle exposures, blood pressure, and baseline laboratory tests. Depending on your healthcare system and clinical circumstances, ultrasound may be used for dating, confirming intrauterine pregnancy, or assessing viability, but timing varies.
Accurate dating matters because many screening options are time-sensitive. First-trimester screening, non-invasive prenatal testing, and nuchal translucency ultrasound are typically discussed around this period or the coming weeks, depending on local guidelines and individual risk factors. These tests are screening tools, not definitive diagnoses, unless followed by diagnostic testing when indicated.
This is also an opportunity to review medication safety. Do not stop or start prescription medicines, herbal products, or high-dose supplements without professional advice, particularly if you take treatments for epilepsy, hypertension, diabetes, thyroid disease, mental health conditions, autoimmune disease, or clotting disorders. The safest plan is individualized and balances fetal development with the health of the pregnant person.
Nutrition and daily habits that support early fetal development
During week 9, the fetus is small, so caloric needs may not increase dramatically for most people, but micronutrient quality matters. Folic acid or folate remains important for neural development, and prenatal vitamins often include iron, iodine, vitamin D, and other nutrients depending on regional recommendations. Your clinician can advise on the appropriate supplement formulation, especially if you have anemia, a restricted diet, malabsorption, prior bariatric surgery, or thyroid disease.
Practical supportive habits include:
- Eating small, frequent meals if nausea makes large meals difficult
- Prioritizing protein, complex carbohydrates, healthy fats, fruits, vegetables, and adequate hydration
- Avoiding alcohol and discussing smoking, vaping, or substance use support without shame
- Following food safety advice, including caution with unpasteurized products, undercooked meats, and high-mercury fish
- Continuing gentle physical activity if approved and comfortable, such as walking or prenatal-appropriate movement
If eating is difficult, aim for realistic harm reduction rather than perfection. A few days of bland foods during nausea is common. However, if you cannot keep fluids down, urinate very little, feel dizzy, or are losing weight, seek medical care because treatment may be needed.
Emotional health in the first trimester
The beginning of the fetal stage can bring relief, excitement, fear, or all of these emotions at once. Many people are still keeping the pregnancy private at week 9, which can make symptoms and worries feel isolating. If you have a history of miscarriage, infertility treatment, traumatic birth, anxiety, depression, or medical complications, this week may feel especially emotionally loaded.
Emotional health is part of prenatal health. Consider telling one trusted person if secrecy is increasing your stress, or ask your healthcare team about mental health resources. Persistent panic, hopelessness, inability to function, intrusive thoughts, or thoughts of self-harm need urgent professional support. Pregnancy does not protect against mental health conditions, and effective help is available.
Seek urgent medical advice if you experience
- Heavy vaginal bleeding, passing clots, or bleeding with significant cramping
- Severe or one-sided pelvic or abdominal pain, shoulder-tip pain, fainting, or dizziness
- Persistent vomiting with inability to keep fluids down or signs of dehydration
- Fever, chills, painful urination, or symptoms suggesting infection
- Severe headache, visual changes, chest pain, shortness of breath, or sudden swelling
- Thoughts of self-harm, feeling unsafe, or severe emotional distress
Tools & Assistance
- Book or confirm your first prenatal appointment with a midwife, obstetrician, or qualified pregnancy care provider
- Prepare a list of current medications, supplements, allergies, medical conditions, and family history for your visit
- Use a pregnancy-safe symptom diary to track nausea, bleeding, pain, mood, hydration, and questions for your clinician
- Ask your healthcare team about first-trimester screening options and timing
- Contact urgent care, emergency services, or your maternity triage line if warning signs occur
FAQ
Is the baby an embryo or a fetus at 9 weeks?
Many references describe week 9 as the start of the fetal stage. The major body plan is established, and development now focuses on growth, maturation, and refinement of organs and structures.
Can I feel fetal movement at 9 weeks?
No, movement is usually not felt this early. The fetus may make spontaneous movements, but it is still too small for those movements to be perceived.
Is it normal for pregnancy symptoms to change from day to day?
Yes. Nausea, breast tenderness, fatigue, and mood symptoms can fluctuate. However, heavy bleeding, severe pain, fainting, fever, or persistent vomiting should be assessed by a healthcare professional.
How big is the fetus at week 9?
Measurements vary by method and dating. The NHS describes the fetus as about 22 mm long, roughly the size of a strawberry, while other sources may report different crown-rump length estimates.
Should I have an ultrasound at 9 weeks?
Some people have an ultrasound around this time, while others do not until later. The need and timing depend on local practice, symptoms, dating uncertainty, medical history, and your clinician’s recommendation.
Sources
- National Health Service (NHS) — 9 weeks pregnant guide - Best Start in Life - NHS
- American Pregnancy Association — 9 Weeks Pregnant
- Charlotte Lozier Institute — Week 9
Disclaimer
This article is for informational purposes only and does not replace individualized medical advice, diagnosis, or treatment. Always consult a qualified healthcare professional about pregnancy symptoms, medications, tests, or concerns.