Intro
Week 14 of pregnancy often feels like a meaningful threshold. You are entering the early second trimester, and for many people this period brings a gradual easing of first-trimester symptoms, a little more energy, and growing curiosity about what the baby is doing inside the uterus. At this stage, fetal development is increasingly dynamic: muscles and nerves are coordinating more efficiently, limbs are moving, and the face is becoming more expressive and proportionate.
Although most pregnant people cannot yet feel fetal movements at 14 weeks, movement is already happening. The baby may kick, stretch, flex tiny joints, and make facial movements as neuromuscular pathways mature. These early actions are not usually under conscious control; they are part of the complex developmental process that helps muscles, nerves, bones, and joints mature together.
Highlights
At 14 weeks, the fetus is already moving, kicking, and flexing, even though these movements are usually too small to be felt.
Facial development is advancing, with more defined features and early movements involving the mouth, eyes, and facial muscles.
Muscle and nerve maturation are closely linked; movement helps support coordinated growth of limbs and joints.
The baby’s body is becoming more proportionate as the head growth slows relative to the rest of the body.
Symptoms and experiences vary widely at this stage, so individualized guidance from a midwife, obstetrician, or other healthcare professional remains important.
Your baby at week 14: small, active, and changing quickly
At 14 weeks of pregnancy, fetal development has moved beyond the earliest organ-forming phase and into a period of rapid growth and refinement. The fetus is still very small, but the body is becoming more coordinated and proportionate. The head remains relatively large, yet growth of the trunk and limbs is helping the overall shape look increasingly like a newborn in miniature.
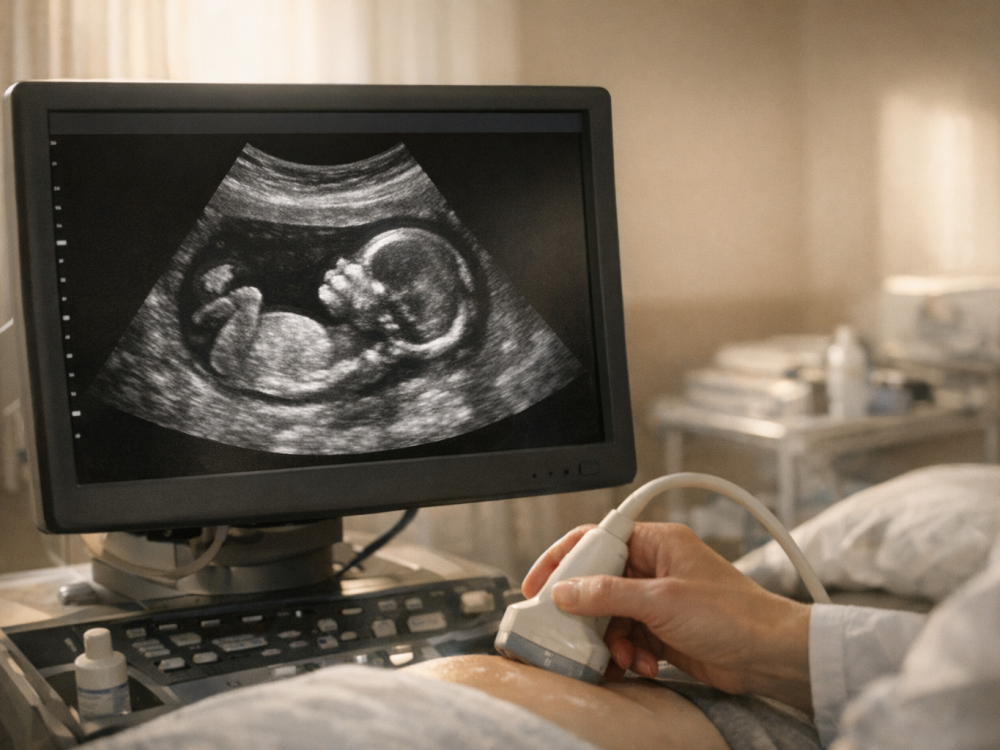
The second trimester is often described as a time when fetal movements become more organized. The nervous system continues to mature, and muscles are developing enough to create visible movements on ultrasound. These may include stretching, bending the arms and legs, turning, or making brief jerky motions. The pregnant person usually does not perceive these movements yet because the fetus is still small, the movements are light, and the uterine wall, amniotic fluid, and placenta all buffer sensation.
It is natural to wonder whether not feeling anything means something is wrong. At week 14, the answer is usually no. Feeling fetal movement, sometimes called quickening, typically occurs later, often around 16 to 24 weeks, depending on factors such as whether this is a first pregnancy, placental position, body habitus, and individual sensitivity. If you have specific concerns, especially if symptoms change suddenly, it is always appropriate to contact your maternity care team.
Early fetal movements: what is happening before you can feel it
Fetal movement begins well before it becomes noticeable to the pregnant person. By week 14, the baby may be kicking, moving the arms, turning the head, and flexing at the wrists, elbows, knees, and ankles. These movements are generated by developing muscles and increasingly connected neural pathways. They are an important sign of neuromuscular maturation, but they are not the same as purposeful movement in an older infant.
These early motions can appear spontaneous and irregular. They may be influenced by the maturation of the spinal cord, brainstem, peripheral nerves, and muscle fibers. As the fetus grows, the movements gradually become stronger and more coordinated. Ultrasound may capture these motions, although a brief scan may or may not show dramatic activity at a given moment because fetal activity cycles vary.
- Small limb movements may include flexion and extension of arms and legs.
- The fetus may turn or make whole-body shifts within the amniotic fluid.
- Hands may move toward the face, and fingers may flex as small muscles develop.
- Movements are usually not felt at this stage, especially in a first pregnancy.
For many people, waiting to feel movement can be emotionally intense. It may help to remember that lack of perceived movement at 14 weeks is expected and not, by itself, a warning sign. Later in pregnancy, your care team will give you guidance about fetal movement awareness and when changes should be assessed.
Facial development: features, expressions, and tiny reflexes
Week 14 is also a fascinating time for facial development. The eyes have moved closer toward the front of the face compared with earlier weeks, the ears are moving toward their more typical position, and the nose, jaw, and mouth continue to refine. The face is not fully mature, but its proportions and contours are becoming more recognizable.
Facial muscles are developing alongside the nerves that supply them. This means the fetus may begin making subtle facial movements. These can include opening and closing the mouth, moving the lips, or making small movements that resemble grimacing or frowning. Such expressions are developmental motor patterns rather than emotional expressions as we understand them after birth.
Swallowing movements also begin to become more relevant during this phase of pregnancy. The fetus is surrounded by amniotic fluid and may practice swallowing small amounts. These repetitive actions contribute to the maturation of the gastrointestinal tract and neuromuscular coordination. Similarly, early mouth and jaw movements support the gradual development of structures that will later be involved in sucking and feeding.
It can be moving to imagine a tiny face becoming more defined each day. At the same time, it is important not to overinterpret a single ultrasound image or facial position. Fetal posture, angle, movement, and imaging limitations can all affect what appears on a scan.
Muscle and nerve development: building the movement system
Muscle development at 14 weeks is closely connected to the maturation of the fetal nervous system. Skeletal muscles, which attach to bones and enable voluntary movement after birth, are developing in size and function. Nerve signals stimulate muscle contractions, and repeated contractions help shape motor pathways. This reciprocal relationship between nerves and muscles is essential for normal movement development.
Early fetal movement also supports skeletal and joint development. When limbs move in the amniotic fluid, the mechanical activity contributes to joint formation, muscle tone, and bone modeling. The fetus is not exercising in the adult sense, but movement is still biologically meaningful. The uterus provides a buoyant environment where motion can occur with minimal gravitational load.
Coordination remains immature. Movements can be sudden, start-and-stop, or asymmetrical. Over time, as the cerebral cortex, brainstem, spinal cord, and peripheral nerves mature, movements become more patterned. Later in pregnancy, the baby may develop cycles of activity and rest that become recognizable to the pregnant person.
If you have a prenatal scan around this period, you may see brief movements that look surprisingly lively. If you do not see much movement during a scan, that does not automatically mean there is a problem. Fetal position, timing, equipment, and the purpose of the scan all matter. Your clinician or sonographer is the best person to interpret findings in context.
Changes you may notice in your own body
As the placenta continues to support the pregnancy and hormone patterns shift, many people begin to feel some relief from nausea and profound fatigue, though this is not universal. Some continue to experience vomiting, food aversions, breast tenderness, constipation, headaches, nasal congestion, or mood changes. Others feel more energetic but notice new sensations such as stretching, pulling, or mild cramping as the uterus grows.
The uterus is rising out of the pelvis, and your abdomen may begin to look or feel different. Whether you appear visibly pregnant at 14 weeks varies widely. Factors include body shape, abdominal muscle tone, previous pregnancies, bloating, and the position of the uterus. There is no single correct appearance at this stage.
Round ligament discomfort can begin for some people as the ligaments supporting the uterus stretch. This is often described as a brief sharp or pulling sensation in the lower abdomen or groin, especially with position changes. However, abdominal or pelvic pain should not automatically be assumed to be benign. Severe pain, persistent pain, pain with bleeding, fever, dizziness, shoulder-tip pain, or feeling faint should be assessed promptly.
Emotionally, week 14 can bring relief, anxiety, or both. After the first [[mamaspedia_link:86|trimester]], some people feel more confident, while others remain cautious, especially after previous pregnancy loss, fertility treatment, or medical complications. Your emotional response is valid. If anxiety feels overwhelming or interferes with sleep, appetite, or daily functioning, consider discussing it with a healthcare professional.
Prenatal care and screening around week 14
Care at this stage depends on your location, medical history, and earlier test results. Some people have already had first-trimester screening, dating ultrasound, or blood tests. Others may be preparing for second-trimester screening or follow-up appointments. Your clinician may review blood pressure, weight trends, symptoms, medications, supplements, and any risk factors that require individualized monitoring.
If prenatal genetic screening is part of your care plan, timing matters. Some screening tests are performed in the first trimester, while others occur in the second trimester. Screening tests estimate risk; they do not diagnose most fetal conditions. Diagnostic tests, such as chorionic villus sampling or amniocentesis, involve different timing, indications, benefits, and risks. Decisions about testing are personal and should be made with qualified medical counseling.
You may also discuss nutrition, physical activity, sleep, work exposures, travel, vaccinations, and mental health. Many people continue taking a prenatal vitamin that includes folic acid, and some may need iron, vitamin D, iodine, calcium, or other supplementation depending on diet, laboratory findings, and local guidance. Do not start high-dose supplements or herbal products without medical advice, as some can be inappropriate in pregnancy.
If you have chronic conditions such as hypertension, diabetes, thyroid disease, epilepsy, autoimmune disease, kidney disease, or a history of clotting disorders, week-by-week guidance may differ. Medication adjustments should always be handled by a clinician; stopping prescribed medication suddenly can be harmful.
Supporting healthy development without trying to control everything
It is understandable to want to do everything perfectly, especially when fetal development feels both miraculous and fragile. The most helpful approach is usually consistent, evidence-informed care rather than perfection. Regular prenatal visits, balanced nutrition, appropriate activity, avoidance of known harmful exposures, and timely attention to symptoms all support a healthy pregnancy.
- Attend scheduled prenatal appointments and ask questions when something is unclear.
- Follow your clinician’s advice about prenatal vitamins, screening, and management of existing conditions.
- Avoid alcohol, smoking, recreational drugs, and non-prescribed medications unless a healthcare professional has confirmed safety.
- Choose physical activity that is appropriate for your pregnancy and medical history.
- Seek support for emotional distress, relationship concerns, or practical needs.
You do not need to feel fetal movement yet to bond with your baby. Some people talk to the baby, journal, look at ultrasound images, or simply take quiet moments to acknowledge the pregnancy. Others feel detached or cautious, and that can also be normal. Bonding is not a test you have to pass; it develops differently for everyone.
When to seek medical advice promptly
- Vaginal bleeding, fluid leakage, or severe pelvic or abdominal pain should be assessed urgently.
- Contact a healthcare professional for fever, fainting, severe dizziness, or persistent vomiting.
- Pain with shoulder-tip discomfort, collapse, or feeling very unwell needs urgent evaluation.
- Do not wait for fetal movement at 14 weeks as reassurance; it is usually too early to feel it reliably.
- Speak with your maternity team before changing prescribed medications or starting supplements.
Tools & Assistance
- Prenatal appointment checklist for symptoms, medications, and questions
- Local maternity triage or obstetric advice line
- Pregnancy-safe medication review with a pharmacist or clinician
- Ultrasound and screening schedule from your prenatal care provider
- Mental health support service for pregnancy-related anxiety or low mood
FAQ
Can I feel my baby move at 14 weeks?
Usually not. The fetus is moving, but the movements are typically too small and light to be felt. Many people notice first movements later, often between 16 and 24 weeks.
What kind of facial development is happening now?
Facial features are becoming more defined, and small muscles may create early mouth, lip, and facial movements. These are developmental motor patterns, not emotional expressions.
Is it concerning if an ultrasound does not show much movement?
Not necessarily. Fetal activity varies, and a short scan may capture a quiet moment or a difficult angle. Your sonographer or clinician should interpret findings in context.
Why are muscles important at this stage?
Developing muscles work with nerves to create early movements. These movements support joint, bone, and neuromuscular development as the fetus grows.
Should I change my exercise routine in week 14?
Many people can continue appropriate pregnancy-safe activity, but recommendations depend on your health, pregnancy risk factors, and previous activity level. Ask your healthcare professional for individualized advice.
Sources
- Mayo Clinic — Fetal development: The second trimester
- NHS — Fetal development week by week
- MedlinePlus — Development of the Fetus: MedlinePlus Medical Encyclopedia
Disclaimer
This article is for informational purposes only and does not replace medical advice, diagnosis, or treatment. Always consult your midwife, obstetrician, or healthcare professional about personal pregnancy concerns.