Intro
Week 16 of pregnancy sits in the early-to-middle part of the second trimester, a time when many people notice that pregnancy begins to feel more physically real. The uterus is rising out of the pelvis, routine prenatal visits may include discussion of fetal growth and screening results, and the fetus is entering a phase of rapid size gain and increasingly organized movement.
At this stage, development is not only about becoming larger. The fetal nervous system, muscles, skeleton, heart, and blood vessels are working together with growing precision. Movements that began as tiny reflexive twitches are becoming more coordinated, circulation is supporting fast tissue growth, and ultrasound may show limb activity even before you reliably feel movement yourself.
Highlights
At around 16 weeks, the fetus is growing quickly and may increase substantially in size over the coming month.
Limb movements are becoming more coordinated as the brain, spinal cord, muscles, and joints mature together.
The fetal heart and circulation are already highly active, supporting oxygen and nutrient delivery through the placenta.
Some pregnant people begin to sense early fetal movement around this period, but many do not feel it until later, especially in a first pregnancy.
Week 16 is often a good time to review prenatal screening, nutrition, symptoms, and upcoming ultrasound plans with a healthcare professional.
Fetal size at week 16: small, active, and growing fast
By week 16, fetal size is commonly compared to a small avocado, though individual measurements vary. Reference data commonly place the average fetus at roughly 11 to 12 centimeters crown-to-rump length, with a weight near 100 grams. These numbers are approximations rather than performance targets; fetal position, dating accuracy, parental body size, and ultrasound measurement technique can all influence estimates.
The key developmental theme this week is acceleration. Public-health pregnancy guidance notes that the fetus is growing quickly at 16 weeks and may soon double in size over the next month. This rapid growth is supported by increased placental function, expanding blood volume, skeletal mineralization, and ongoing organ maturation.
At this stage, fetal proportions are also changing. The head remains large compared with the body, but the torso and limbs are lengthening. The neck is more defined, the legs are becoming longer relative to the arms, and facial features are becoming more recognizable. These structural changes create the physical basis for more visible, coordinated fetal movement.
Coordination: how movement becomes more organized
Fetal begins well before a pregnant person can usually feel it. By week 16, the nervous system is developing more refined connections between the brain, spinal cord, peripheral nerves, and muscles. Mayo Clinic notes that around this point limb movements are becoming coordinated and may be visible on . This means the fetus may flex and extend the arms and legs, bring hands toward the face, or change posture in ways that look more purposeful than earlier reflexive motions.
Coordination does not mean voluntary movement in the adult sense. Rather, it reflects maturing neuromuscular circuitry. Motor neurons stimulate muscle fibers; joints allow range of motion; the skeleton provides leverage; and sensory input begins to shape repeated movement patterns. These rehearsals are important for musculoskeletal development, joint mobility, and later motor function.
Some people describe early fetal movement as fluttering, bubbles, tapping, or a faint rolling sensation. This is often called quickening. It may start around 16 to 20 weeks, but timing is highly variable. People who have been pregnant before may recognize it earlier, while those with a first pregnancy, a placenta positioned at the front of the uterus, or a higher body mass index may notice movement later. Not feeling movement at exactly 16 weeks is usually not, by itself, a sign of a problem, but any concern should be discussed with a maternity care professional.
Eyes, ears, and sensory-motor development
Week 16 also brings important sensory milestones that contribute indirectly to coordination. According to Mayo Clinic, the eyes can move slowly, even though the eyelids remain closed. Eye movement reflects maturation of cranial nerves and brainstem pathways, and it is one small sign of increasing neurologic complexity.
The ears are nearing their final position on the sides of the head. Hearing-related structures continue to mature, and while responses to sound become more clinically meaningful later, the anatomic groundwork is being laid. The fetus is surrounded by maternal body sounds, including heartbeat, blood flow, bowel activity, and voice vibration. These acoustic experiences occur in a fluid environment and are filtered by maternal tissues, so they are very different from hearing after birth.
Facial muscles are also developing. The fetus may make small facial movements, swallow amniotic fluid, and practice motions that will later support feeding and breathing adaptation after birth. These activities are not conscious behaviors; they are al exercises coordinated by emerging neuromuscular pathways.
Fetal circulation: the placenta as life-support system
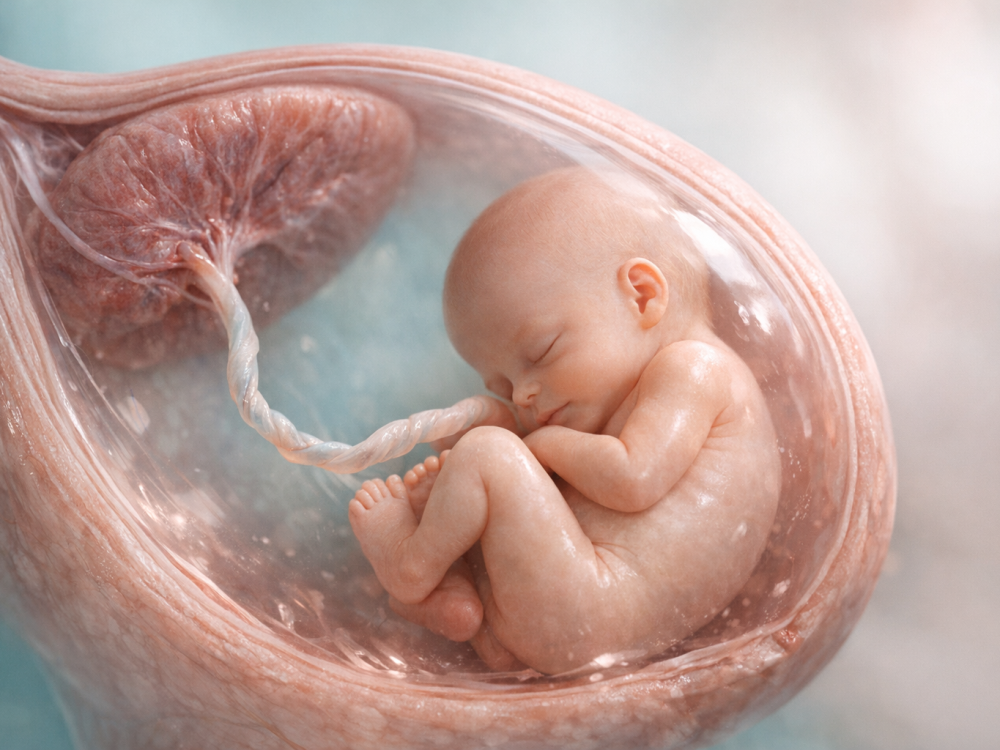
By week 16, fetal circulation is well established and highly specialized for life inside the uterus. Unlike after birth, fetal lungs are not yet responsible for oxygen exchange. Oxygen and nutrients come through the placenta, an organ that interfaces with maternal blood supply while maintaining separate maternal and fetal circulations.
Oxygenated blood travels from the placenta to the fetus through the umbilical vein. Fetal circulation then prioritizes the brain, heart, and upper body through unique pathways, including the ductus venosus, foramen ovale, and ductus arteriosus. These shunts are normal fetal structures that help route blood efficiently before the lungs are functioning as air-breathing organs. After birth, changes in lung expansion, oxygen levels, and vascular resistance trigger major circulatory transitions.
The fetal heart is already beating vigorously and has been doing so for many weeks. During prenatal visits, a clinician may be able to detect fetal heart activity with Doppler ultrasound, depending on gestational age, fetal position, uterine anatomy, and equipment. A single heart rate value should be interpreted only in clinical context; if a measurement is difficult to obtain or seems unexpected, the appropriate next step is professional assessment rather than self-interpretation.
Growth coordination between placenta, blood volume, and maternal physiology
Fetal growth at 16 weeks depends on close coordination between maternal physiology, placental function, and fetal cardiovascular development. Maternal blood volume expands during pregnancy, cardiac output rises, and the uterus receives increasing blood flow. These adaptations help deliver oxygen, glucose, amino acids, fatty acids, micronutrients, and hormones to the placenta.
For the pregnant person, these circulatory changes can produce noticeable sensations. Some people feel warmer, more easily breathless with exertion, lightheaded when standing quickly, or aware of a faster heartbeat. Mild changes can be part of normal adaptation, but symptoms such as fainting, chest pain, severe shortness of breath, persistent palpitations, or one-sided leg swelling should be assessed promptly.
Nutrition also matters, but it does not require perfection. Iron, folate, iodine, vitamin D, calcium, protein, and omega-3 fatty acids may all be discussed in prenatal care depending on diet, medical history, local guidance, and lab results. Supplements should be chosen with a healthcare professional, especially if there are medical conditions, anemia, thyroid disease, gastrointestinal disorders, medication interactions, or a history of pregnancy complications.
What you may notice in your body at 16 weeks
Many people feel somewhat better in the second as nausea and fatigue improve, though this is not universal. The uterus may be more noticeable above the pubic bone, and clothing may fit differently. Round ligament discomfort, mild pelvic pulling, nasal congestion, constipation, heartburn, breast changes, and skin pigmentation changes can occur.
Emotionally, week 16 can be a mixed point. Some people feel relief after early pregnancy uncertainty; others feel anxious while waiting for screening results, anatomy ultrasound scheduling, or the first unmistakable fetal movements. Both reactions are understandable. Pregnancy is a physiologic process, but it is also a major psychological and social transition.
Helpful discussion topics for a prenatal appointment around this time may include:
- Whether gestational dating is confirmed and how fetal will be monitored
- Results or options for aneuploidy screening, carrier screening, or serum screening if relevant
- Timing of the mid-pregnancy anatomy ultrasound, commonly performed later in the second trimester
- Medication safety, including over-the-counter drugs and herbal products
- Exercise, work demands, travel, sleep position, and symptom management
Ultrasound at 16 weeks: what might be seen
If an ultrasound is performed at or near 16 weeks, fetal movement may be visible even if it is not yet felt. The fetus may stretch, turn, flex limbs, or bring hands near the mouth. Depending on the indication for the scan, a clinician or sonographer may evaluate fetal heartbeat, number of fetuses, placental location, amniotic fluid, fetal biometry, and selected anatomy.
Sex-related anatomy may sometimes be suggested around this stage, but accuracy depends on fetal position, image quality, gestational age, and operator experience. The more detailed structural evaluation is typically the mid-trimester anatomy scan, often scheduled around 18 to 22 weeks depending on local practice.
It is wise to avoid overinterpreting keepsake ultrasound images or non-medical scans. Ultrasound is a medical imaging tool, and findings should be explained by qualified professionals who can connect images with gestational age, medical history, and appropriate follow-up.
When to seek medical advice promptly
- Vaginal bleeding, fluid leakage, or severe cramping should be discussed with a healthcare professional urgently.
- Severe headache, visual changes, chest pain, fainting, or significant shortness of breath needs prompt assessment.
- Fever, painful urination, persistent vomiting, or signs of dehydration should not be ignored.
- One-sided calf pain, swelling, redness, or sudden breathlessness may require urgent evaluation.
- If something feels wrong or symptoms are escalating, contact your maternity unit, clinician, or emergency service according to local guidance.
Tools & Assistance
- Schedule or confirm your next prenatal visit
- Prepare questions about fetal growth, movement, screening, and the anatomy ultrasound
- Keep a symptom note to discuss with your midwife, obstetrician, or family physician
- Review medications, supplements, and herbal products with a healthcare professional
- Use trusted public-health pregnancy resources rather than non-medical forums for clinical decisions
FAQ
How big is the fetus at 16 weeks?
Average estimates are about 11 to 12 centimeters crown-to-rump length and around 100 grams, but normal variation is expected. Your clinician can interpret measurements in context.
Should I feel fetal movement at week 16?
Some people do, especially in a later pregnancy, but many do not feel clear movement until 18 to 20 weeks or later. Ask your healthcare professional if you are worried.
What does coordinated movement mean at this stage?
It means the fetal nervous system, muscles, joints, and skeleton are maturing enough for more organized limb activity, often visible on ultrasound.
Is the fetal circulation the same as a newborn’s circulation?
No. Before birth, oxygen exchange occurs through the placenta, and fetal blood uses specialized shunts that help route circulation efficiently until the lungs take over after birth.
Can ultrasound at 16 weeks detect all problems?
No. Ultrasound can provide valuable information, but some findings are not visible this early or may require later imaging, specialist review, or additional testing.
Sources
- Mayo Clinic — Fetal development: The 2nd trimester
- Pregnancy, Birth and Baby — Pregnancy at week 16
- Perinatology.com — Fetal Development
Disclaimer
This article is for general educational information and is not a substitute for individualized medical advice, diagnosis, or treatment. Always consult your doctor, midwife, or qualified healthcare professional about pregnancy symptoms, test results, and care decisions.